
Donor Support Helps Turn Passion Into Patient Care
“I just want to give a huge thank you. Most donors do not even know who they are helping, but they are still investing in

“I just want to give a huge thank you. Most donors do not even know who they are helping, but they are still investing in
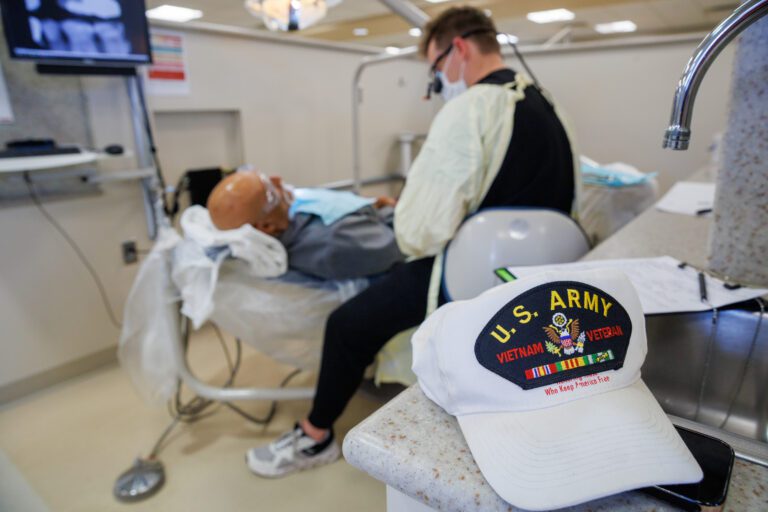
“What we’re doing couldn’t be done any other way. This program couldn’t exist, and without this program, these people will not receive definitive, life-changing care.”

“It’s so nice for students to have something outside the classroom, even if it is directly tied to what they’re going to school for.”

“The College of Pharmacy Innovation Fund continues to be a vital source of support for our students, faculty and the UNMC Alumni Association. These collective

“I just want to thank donors for their support to this fund. You have made it possible to have such an inclusive environment where students

“A student organization is going to be impacted, not just in that moment, but for years down the road. We see student organizations that come

“I’m really grateful for all the support I’ve had, whether it’s been from my family, my professors, or the financial help through scholarships. It makes

The College of Pharmacy Innovation Fund isn’t just an educational resource — it’s a living, breathing network that continues to shape the future of pharmacy,

The Wellness Hub is the center point for students to receive the support they are looking for.

“Thanks to the doctors like Dr. Lunning and the entire staff at Nebraska Medicine, I’ve been given another decade with my husband.”